SUBCOSTAL TAP
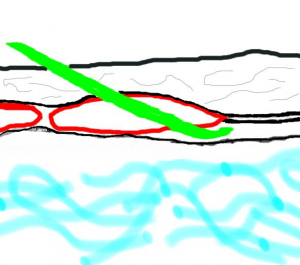 As I mentioned in the previous section, I believe that the subcostal TAP block is even easier than the TAP block. With the TAP block, the main difficulty is getting within (or just below or above) the fascial plane without puncturing the bowel. This can involve a significant amount of scraping or jabbing type of movements that makes one anxious only a few centimeters from the bowels. The subcostal approach offers a ‘free pass’ to the desired location as soon as you pass through the rectus muscle just under the xiphoid process. The aponeurosis just below your needle is that of the transversus abdominus muscle. (The T.A. aponeurosis joins under the medial aspect of the rectus muscle, and the I.O. aponeurosis joins at the lateral border of the rectus muscle.) You now only need to hydrodissect your way in an oblique orientation along the border of the rib margin toward the typical needle insertion site for a TAP block. You do need to attempt to pierce the posterior border of the rectus muscle closer to the lateral border before the aponeurosis of the transversus abdominus adheres to the posterior border of the rectus muscle to optimize the safety profile of this block. In the lateral aspect of the muscle, the needle will easily enter the space between the aponeurosis of the transversus abdominus and internal oblique with little risk of piercing the transversus abdominus aponeurosis.
As I mentioned in the previous section, I believe that the subcostal TAP block is even easier than the TAP block. With the TAP block, the main difficulty is getting within (or just below or above) the fascial plane without puncturing the bowel. This can involve a significant amount of scraping or jabbing type of movements that makes one anxious only a few centimeters from the bowels. The subcostal approach offers a ‘free pass’ to the desired location as soon as you pass through the rectus muscle just under the xiphoid process. The aponeurosis just below your needle is that of the transversus abdominus muscle. (The T.A. aponeurosis joins under the medial aspect of the rectus muscle, and the I.O. aponeurosis joins at the lateral border of the rectus muscle.) You now only need to hydrodissect your way in an oblique orientation along the border of the rib margin toward the typical needle insertion site for a TAP block. You do need to attempt to pierce the posterior border of the rectus muscle closer to the lateral border before the aponeurosis of the transversus abdominus adheres to the posterior border of the rectus muscle to optimize the safety profile of this block. In the lateral aspect of the muscle, the needle will easily enter the space between the aponeurosis of the transversus abdominus and internal oblique with little risk of piercing the transversus abdominus aponeurosis.
Once I have passed through the rectus muscle with a six inch Tuohy needle, I will have my assistant inject a few mls of local anesthetic to hydrodissect, then I will advance my needle under ultrasound guidance, and we just continue this pattern until I have gone as far as the needle will take me. Once you have gone as far as you are able, just thread the catheter to the end of the needle and withdraw the needle. Some will use saline during this process in order to avoid using too much local anesthetic, then they will bolus afterward with local. I don’t find the need for this, and it adds more time to doing the block (and likely increases the time of onset as well). I use concentrations between 0.2% ropivicaine or 0.375% bupivicaine (with or without 1:400,000 epi) depending whether I am adding bilateral TAPS (or doing only one subcostal TAP like if there is a colostomy in the way, for example), and I make sure my assistant is aware of the volume to be injected so I don’t accidentally run out of local too soon. I ask them to alert me at 1/4, 1/2, and 3/4 of the volume just in case. When I get done, I have them inject the rest through the needle before I insert the catheter. It may create a better distribution of local along the catheter due to ‘track back’ to inject any remaining volume through the catheter, but that adds valuable time to the procedure (That is, it is easier and faster to inject through a large bore Tuohy than a catheter, and, remember, you have to do the same on the other side. Also, the higher bolus pressure through the needle may extend the pocket of local further which may increase the area covered by the block in the end. I have seen bubbles of air at the iliac crest after doing the subcostal TAP as I’ve prepared to do the TAP on the same side, so I don’t add the TAP unless the incision significantly beyond the navel.
There are a few issues to keep in mind with this block. The first is about the timing of catheter placement. Commonly, this block is performed post-operatively in the O.R. while the patient is still under a general anesthetic. It is much harder (if not impossible) to do this after their dressings have been placed, so make sure you have everything ready to go and that you are adequately warned about the time of closing. If the plan is to place the block at the end of the case (in the O.R. or in the PACU), the opioid management has to be discussed. If it is estimated that the patient has received enough long-acting opioid to cover their post-operative pain, then bolusing the catheters may need to be done at a later time or just plan to only initiate an infusion. The other strategy (this is what we do) would be to use short-acting opioids intraoperatively, and bolus the catheters when they are placed at the end of surgery. If the patient is still expected to go to the intensive care unit intubated, then the issue is not as pressing (Hopefully, this block will decrease the number of patients that do stay intubated!). I like the anesthetist to ‘get the patient breathing’ at the end of the case to ‘see where we are starting’ and plan the post-operative course accordingly. Once they have done this, I have them ‘over-breath’ the patient with the ventilator. It is an enormous challenge to try to advance the needle between breaths with the obliques flexing. It is like suddenly doing the block in the open ocean when they are breathing on their own. This literally tripled the time it used to take me to do this block!
Another issue is whether or not bilateral TAP blocks (single or continuous) are going to be utilized. There is evidence that supplementing for the caudal aspect of the incision may not be necessary. Certainly, the worst pain will come from the cranial aspect of the incision, so this would be the most important aspect to cover if one had to choose between the two blocks. I have commonly used the strategy of two continuous subcostal TAP blocks along with two single injection TAP blocks for an exploratory laparotomy. I had started out using four catheters, placing the TAP catheters ahead of time whenever possible. I would hook the subcostals to infusions, and bolus intermittently the TAPs if at all. This, I found to be too cumbersome unless the incision extends to the pubis. Now, the common ‘4 block scenario’ occurs when a low incision for a sigmoid colectomy gets extended significantly above the navel for some reason. (If it only extends to just above the navel, I do continuous TAP blocks ‘relatively high’ but being sure to keep my catheter adjacent to the II/IH nerves).
I have recently switched to[nonmember]…
REGISTER for FREE to become a SUBSCRIBER or LOGIN HERE to see the full article!
[/nonmember]
[ismember] using continuous bilateral subcostal blocks plus or minus bilateral single injection TAP’s. I stumbled onto my last strategy when I found that the ‘step up’ in pain when I expected the TAP blocks to wear off was minimal or never happened. Because of this, it might be reasonable to place bilateral continuous subcostal TAP blocks and skip the TAP block completely (or place single injections as a rescue block if needed) if we get far enough with the subcostal block. So, see how the subcostal blocks go, and decide whether to add the TAP blocks at that point. Another reason to go in this order if you do choose to do all four catheters is so you don’t run over your dressing (obscures ultrasound view) or dislodge (or get gel all over) the catheter if it isn’t yet dressed. If you do have trouble extending the subcostal TAP block, try to hydrodissect from the typical TAP block location cranially and medially (instead of laterally) along the costal border as this may be another way to ‘bridge the gap’ between the two locations.
To extend my subcostal TAP blocks farther in a caudal direction, I have found two tricks that have become very helpful. First, I ‘aim’ medial to, not toward, the iliac crest. Visualize the actual path ahead of time, and use pressure with your 4th and 5th digits of your probe hand to identify the border of the ribs or extend the butt of your hand to identify the iliac crest and properly orient your planned path without stopping to look. This does two things. It keeps me more over the aponeurosis than the muscle of the transversus abdominus, and it is much easier to hydrodissect here. It can be like hitting a brick wall if you go too far laterally where the muscles are more tightly adherent (If it were easy, I would do subcostal TAP’s starting at the lateral and caudal TAP position and travel cranially!). This also extends the utility of whatever length needle you use. Imagine the needle driving straight down the edge of the rectus muscle, then picture it rotating it laterally. The caudal extent of needle is diminished when it is angled laterally. Do pay attention to retention sutures that the surgeon may have placed when trying to keep medial; you don’t want to inadvertently cut across one of those (though I would imagine you would have to use considerable ‘inappropriate’ force to do so).
The second trick is to bend the needle (see below). I utilize this trick more often when there is significant adipose tissue over the abdomen. When you have to descend through several centimeters of adipose just to get to the rectus muscle, the angle of your needle is more steep of course. As you drive the needle onward, you end up driving it more toward the peritoneum, so angling the needle allows you to ‘make the curve’ much easier. It is fine if this eventually causes your needle to aim in a superficial direction. If this becomes a problem (apart from starting over after decreasing the angle of the bend), you can rotate the needle in a slight medial or lateral direction to minimize the angle. Let me state that bending the needle adds an additional dimension to keeping the needle in-plane with the ultrasound probe.
As I have mentioned, I have been utilizing single injection TAP blocks for exploratory laparotomy incisions, and I maximize the volume bilaterally to this block since this is a single injection. Afterward, I use a low volume of dilute local anesthetic for the Subcostals because they can be supplemented at a later time. This does sound counter-intuitive since, as I mentioned, the worst pain (and respiratory compromise) will come from from the cranial aspect of the incision. Once the patient is awake, if they are hurting at the upper aspect of the incision (and there are no signs of toxicity), the catheter can be further bolused. In my experience, it allows me to use a maximum dose in a way that gives optimal control for the longest period of time where the pain will be the worst.
You certainly have to be aware of the volume and mass of drug used to optimize either of these blocks by allowing enough spread. Further, you need to consider the onset time with respect to the amount and type of opioids used intraoperatively since these blocks are performed later. The advantages to the patient, however, can be significant. Being able to extubate someone after surgery instead of leaving them intubated over night, in addition to being a significant cost-savings to the hospital, can have an enormous impact on their recovery. In a recent case with an elderly patient for an emergency exploratory laparotomy, the patient required no opioids intraoperatively or for the rest of the day. She took one dose of opioids the following day for a headache and remained fully alert and able to deep breathe and cough comfortably. This is someone that I may not have extubated at the end of the case if I had not been able to utilize this treatment. By the way, she went to the floor from the ICU the next morning. My surgeons are taking advantage of these circumstances and are being more aggressive with physical therapy post-operatively.
There are certainly times when a thoracic epidural (or paravertebral blocks) may be the best choice for the patient, however, this comes with a sympathectomy (and hypotension) that can be problematic. Also, coagulation issues and emergency circumstances also preclude the use of this modality. Another advantage of the anterior wall blockade alone is the opportunity for early ambulation with much less concern for falls or hypotension.
Lastly, I have found that unless there is significant retroperitoneal involvement in the surgery, the lack of visceral coverage is rarely of consequence. In fact, recently, I had intended to perform a low continuous paravertebral nerve block for an iliac aneurysm repair that was to be a retroperitoneal approach. Due to equipment issues, I was forced to performed a continuous TAP block. The incision started above the iliac crest laterally and extended under the umbilicus medially. I knew I could cover the anterior wall pain adequately, but I was concerned about the retroperitoneal coverage. Though it turned out to be a major surgery, based on my observations intraoperatively, I requested the surgeon to change his intentions for the patient to go directly to the ICU intubated and allow me to extubate the patient on the table. We were able to do so successfully, and the patient was wide awake in the unit when I visited him that afternoon, and he did not even require supplemental oxygen to maintain 100% oxygen saturation. He took two pain pills through the next day and walked with P.T. around the unit on POD 1. He was transferred to the floor the next morning. There was retroperitoneal involvement, and he had some soreness in his back, but we did not have to use any I.V. opioids. I was happy to be caught off-guard by his exceptional recovery. I have seen many other dramatic differences in analgesia and other beneficial outcomes from the utilization of subcostal blocks.
[/ismember]
See Also: Analgesia for Ex Lap, TAP Block Pain Evaluation